Coronavirus Updates
Mucormycosis (Black Fungus): Frequently Asked Questions
4 min read
By Apollo 24/7, Published on - 28 May 2021, Updated on - 18 October 2022
Share this article
2
25 likes
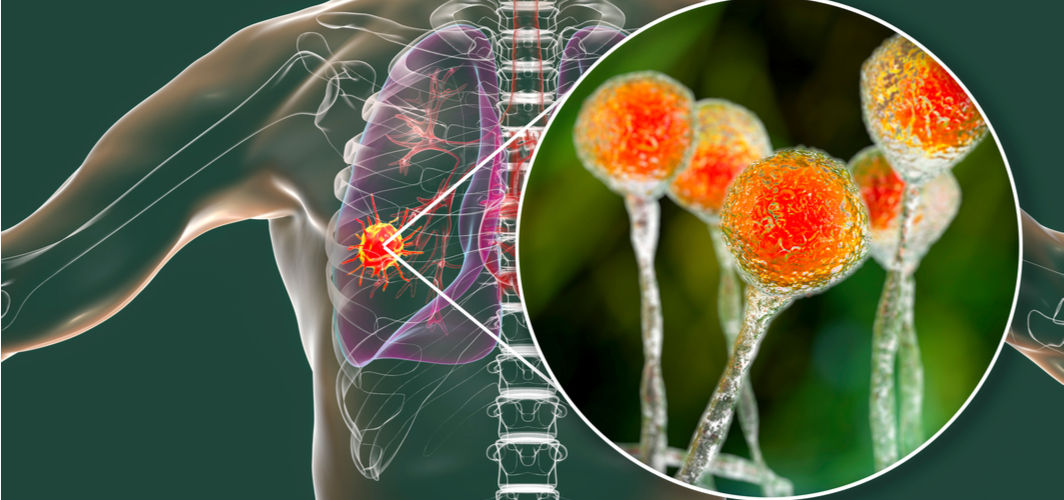
1. What is mucormycosis?
Mucormycosis, or black fungus, is a rare but severe fungal infection. The condition mostly manifests as an invasive rhino-orbito-cerebral disease that affects the eyes, nose, sinuses, lungs, and brain. Without prompt treatment and in rare cases, it can lead to loss of the upper jaw or eye. The mortality rate of mucormycosis ranges between 40% and 80%.
2. What causes mucormycosis?
Black fungus is caused by exposure to a group of molds called mucormycetes. These molds are present throughout the environment but are mostly found in soil and decaying organic matter such as moss, manure, and rotten leaves, vegetables, and fruits. The major routes of exposure include inhaling air contaminated with fungal spores, skin injury, etc.
3. Symptoms of mucormycosis
Some of the most warning signs of mucormycosis include:
- Pain and redness around eyes and/or nose
- Fever
- Headache
- Coughing
- Shortness of breath
- Bloody vomits
- Altered mental status.
4. Who is at risk of mucormycosis infection?
According to the Centers for Disease Control and Prevention (CDC), mucormycosis mainly affects people with health problems or those on medications that reduce their ability to fight germs and sickness. Factors that make a person susceptible to mucormycosis include:
- Diabetes
- Cancer
- Organ transplant
- Stem cell transplant
- Neutropenia (low number of white blood cells)
- Skin injury
- Injection drug use
- Too much iron in the body
- Long term use of corticosteroids and immunosuppressant drugs.
5. What makes COVID-19 patients more susceptible to mucormycosis infection?
According to experts, a complex mix of factors is making hospitalized and recovered COVID-19 patients more susceptible to mucormycosis infection. Uncontrolled diabetes mellitus, immunosuppression by steroids, mechanical ventilation, prolonged stay in ICU, voriconazole therapy, and co-morbidities like cancer and organ transplant are believed to be triggering mucormycosis in COVID-19 patients.
6. When to suspect mucormycosis in hospitalized and recovering COVID-19 patients?
According to the evidence-based advisory for screening, diagnosis, and management of the disease released by the Indian Council of Medical Research (ICMR), mucormycosis infection should be suspected in hospitalized and recovering COVID-19 patients when there is:
- Nasal blockage or congestion
- Blackish or bloody discharge from nose
- Blurred or double vision with pain
- Loosening of teeth
- Appearance of skin lesions
- Thrombosis (formation of clots in veins or arteries)
- Necrosis (death and decaying of tissues)
- Blackish discoloration or lesions on the nasal bridge
- Chest pain and worsening of respiratory symptoms
- Local pain on the cheekbone, one-sided facial pain, numbness or swelling
- Pleural effusion (fluid build-up in the tissues between the lungs and chest cavity).
7. How is mucormycosis diagnosed?
The diagnosis of mucormycosis usually involves collecting samples of fluid from the respiratory system of a suspected patient. The samples are tested in a pathological lab for evidence of fungal infection. The diagnosis process may also include a CT scan of sinuses and lungs or a biopsy of the affected tissue.
8. How to prevent mucormycosis?
Experts say certain precautionary measures can be followed during and after hospitalization (for COVID-19 treatment), to minimize the risk of mucormycosis.
Precautions to be taken during hospitalization:
- Control diabetes and diabetic ketoacidosis
- Stop the use of immunomodulating drugs
- Discontinue use of antifungal medications
- Minimize use of steroids with the aim to discontinue quickly
- Use sterile water for humidification while administering oxygen
- Focus on good oral hygiene with mouthwash and povidone-iodine gargles
Precautions to be taken post-hospitalization:
- Control blood sugar levels
- Stay indoors as much as possible
- Maintain oral and nasal hygiene
- Wear an N-95 mask when going outdoors
- Maintain physical distancing and hand hygiene
- Avoid places with a lot of dust like construction sites
- Avoid activities that involve close contact with soil or manure (such as gardening)
- If this isn’t possible, wear gloves, shoes, long trousers, and long sleeve shirts while handling soil and manure.
9. What are the treatment options for mucormycosis?
According to the ICMR advisory, the medical treatment of mucormycosis may involve:
- Installation of the peripherally inserted central catheter (PICC line)
- Maintenance of adequate systemic hydration
- Infusing normal saline IV before Amphotericin B infusion
- Antifungal Therapy for at least 4-6 weeks.
In most cases, extensive surgical intervention will be eventually required to clear necrotic (decaying) tissue to curb the spread of infection to the brain and other vital organs.
10. What are the long-term prospects for mucormycosis survivors?
In some cases, mucormycosis necessitates surgical intervention that often results in the loss of the upper jaw and sometimes even the eye. Patients would need to come to terms with the loss of function due to a missing jaw or an eye. Prosthetic reconstruction will play a major role in post-surgery rehabilitation. Replacement of the missing facial structures with prosthetics will also ensure the cure is not more dreadful than the disease.
Coronavirus Updates
Leave Comment
Recommended for you

Coronavirus Updates
How to Live With The Coronavirus in this ‘New Normal’
Adapting to and following the new normal is not going to be easy. However, with each other's support and safety protocols in place, we can make the new normal as safe and enjoyable as possible.

Coronavirus Updates
Common Coronavirus Myths and Facts
Seeking the right information from verified sources at a time when we are fighting a pandemic is crucial. You should rely on directives issued by the WHO and MHA for the latest developments about COVID-19.

Coronavirus Updates
What Are the Precautions for Online Shopping During COVID-19?
It is safe to receive online deliveries provided you follow some precautions such as frequent hand washing, physical distancing, and other tips mentioned in this article.
Subscribe
Sign up for our free Health Library Daily Newsletter
Get doctor-approved health tips, news, and more.
Visual Stories

Covid-19 Updates: Are Things Getting Brighter?
Tap to continue exploring
Recommended for you

Coronavirus Updates
How to Live With The Coronavirus in this ‘New Normal’
Adapting to and following the new normal is not going to be easy. However, with each other's support and safety protocols in place, we can make the new normal as safe and enjoyable as possible.

Coronavirus Updates
Common Coronavirus Myths and Facts
Seeking the right information from verified sources at a time when we are fighting a pandemic is crucial. You should rely on directives issued by the WHO and MHA for the latest developments about COVID-19.

Coronavirus Updates
What Are the Precautions for Online Shopping During COVID-19?
It is safe to receive online deliveries provided you follow some precautions such as frequent hand washing, physical distancing, and other tips mentioned in this article.