General Health
Even Non-Alcoholics Are Not Immune to Liver Diseases
5 min read
By Apollo 24|7, Published on - 17 June 2022, Updated on - 11 March 2023
Share this article
0
2 likes

Alcohol is widely believed to be the sole culprit behind liver ailments. However, that is not always the case. It is possible for people to develop liver problems such as non-alcoholic fatty liver disease (NAFLD) without ever consuming alcohol. The article explains the condition in detail below.
What is Non-Alcoholic Fatty Liver Disease?
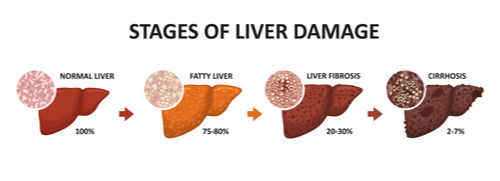
As the name suggests, non-alcoholic fatty liver disease (NAFLD) is a liver condition that is caused by excessive buildup of fat in the liver. It occurs when your liver has over 5 to 10% fat. The changes to the liver caused by NAFLD resemble the damage caused by heavy alcohol intake. In some cases, NAFLD can progress to non-alcoholic steatohepatitis (NASH), a more serious type of fatty liver disease that causes inflammation in the liver. Without treatment and management, the condition can worsen to cause cirrhosis (severe scarring of the liver tissue), and rarely, liver failure.
What are the causes of Non-Alcoholic Fatty Liver Disease?
Researchers are yet to determine the exact cause of non-alcoholic fatty liver disease. They are still studying factors that contribute to the abnormal buildup of fat in the liver. Meanwhile, conditions that may increase the risk for NAFLD include:
- Obesity
- Type 2 diabetes
- High blood pressure
- High cholesterol (Hyperlipidemia)
- High triglycerides (Hypertriglyceridemia)
- Underactive thyroid gland (Hypothyroidism)
- Underactive pituitary gland (Hypopituitarism)
- Polycystic ovary syndrome (PCOS)
- Sleep apnoea
- Metabolic syndrome (a cluster of conditions include hypertension, type 2 diabetes, excess fat around the abdomen, high cholesterol, and elevated triglyceride levels)
What are the symptoms of Non-Alcoholic Fatty Liver Disease?
Non-alcoholic fatty liver disease is often referred to as a silent disease as the condition rarely causes any noticeable symptoms in the beginning. In the majority of the cases, symptoms take years to become evident. Symptoms that may appear include:
- Fatigue or tiredness
- Pain in the upper region of the abdomen
As NAFLD progresses to nonalcoholic steatohepatitis (NASH), the following symptoms may occur:
- Weight loss
- Itchy skin
- Red palms
- Enlarged spleen
- Spider Like blood vessels on the skin
- Enlarged web-like blood vessels just beneath the skin
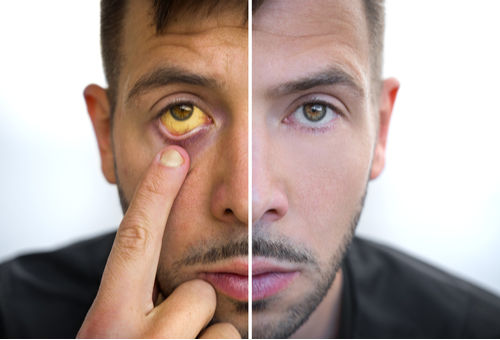
- Jaundice (yellowing of the skin and eyes)
Can Non-Alcoholic Fatty Liver Disease lead to complications?
An untreated case of non-alcoholic fatty liver disease can lead to the inflammation of the liver. When the liver tries to stop inflammation caused by fatty liver, it causes scarring (fibrosis) of the healthy liver tissue. If cirrhosis goes untreated, it may lead to:
- Ascites (accumulation of fluid in the abdominal cavity)
- Oesophagal varices (swelling of the veins in the oesophagus)
- Liver cancer
- Liver failure
How is Non-Alcoholic Fatty Liver Disease diagnosed?
Your physician will look at your medical history to look for factors that may increase your risk of NAFLD. The doctor would also enquire about your diet and lifestyle habits and choices. A physical exam would be done to look for muscle loss, enlarged liver, spleen, and ascites. After the physical exam, your doctor may recommend certain blood tests to look for signs of liver damage:
- CBC (Complete Blood Count) test
- Fasting blood glucose test
- Lipid profile test
- Liver enzyme test
- Hemoglobin A1C (HbA1C) test
- Tests for hepatitis A and C
- Celiac disease screening test
Imaging Tests
- Abdominal ultrasound: The test uses sound waves to produce detailed images of the organs in your abdomen. It is prescribed when your physician suspects liver disease.
- Computed tomography (CT) scan: The imaging test uses x-rays and computer technology to create images of your liver.
- Magnetic resonance imaging (MRI) scan: This test uses radio waves and magnetic fields to produce detailed images of the tissues of the liver.
Elastography is a new diagnostic imaging technique that is primarily used to diagnose advanced liver scarring. It works by measuring the stiffness of the liver tissue, a sign of fibrosis (scarring). Some of the commonly used types of elastography tests are:
- Sheer wave elastography
- Magnetic resonance elastography
- Vibration-controlled transient elastography
Liver Biopsy
When other tests fail to offer conclusive results, your physician may prescribe a liver biopsy (tissue examination) test to check for inflammation and scarring. It involves removing a sample of tissue from the liver which is then sent to a laboratory for analysis. The test is generally recommended only to people who are at increased risk of advanced fibrosis or to those who show signs of liver disease or cirrhosis.
Can NAFLD be prevented?
One can prevent or manage non-alcoholic fatty liver by making certain healthy changes to your diet and lifestyle. Some of those changes include:
- Eat healthy foods: According to research, plant-based diets help improve liver function in patients with NAFLD. Experts recommend eating a plant-based diet that is high in whole grains, vegetables, fruits, nuts, seeds, and fruits for a healthy liver.
- Lose weight: If you are overweight, then consider losing some weight to reduce your risk of NAFLD. Even losing 10% of your body weight can help improve your liver health.
- Exercise regularly: Try to do at least 30 minutes of moderate-intensity exercise daily. Walking, cycling, and swimming are some of the exercises that you can do to reduce your risk of NAFLD.

Non-alcoholic fatty liver disease can cause liver dysfunction in people who don’t consume alcohol. Without timely treatment and lifestyle management, the condition can worsen to cause cirrhosis and liver failure. If you are experiencing any discomfort in your upper abdomen or any of the aforementioned symptoms, it is important to discuss those with an experienced physician to rule out the possibility of NAFLD.
For more information
General Health
Leave Comment
Recommended for you

General Health
5 Most Promising Health Benefits of Taking A Power Nap
Many individuals naturally get more drowsy in the afternoon, roughly 8 hours after waking up. Taking a "power nap" in the middle of the day will improve your health, patience, learning capacity, and efficiency.

General Health
A Complete Guide to Fatigue: Causes, Home Remedies, and Red Flags
Other than a hectic day, fatigue can also happen due to medical reasons! Read this blog, as we highlight the different causes, remedies and red flags of unexplained tiredness and when you should see a doctor.

General Health
Tired All the Time? Tests to Rule Out Underlying Illness
Constantly tired? Discover key blood tests for fatigue—thyroid, B12, Vitamin D, anaemia, and more. Book tiredness test packages online at Apollo 24|7.
Subscribe
Sign up for our free Health Library Daily Newsletter
Get doctor-approved health tips, news, and more.
Visual Stories

Could There Be More to Your Snore?
Tap to continue exploring
Recommended for you

General Health
5 Most Promising Health Benefits of Taking A Power Nap
Many individuals naturally get more drowsy in the afternoon, roughly 8 hours after waking up. Taking a "power nap" in the middle of the day will improve your health, patience, learning capacity, and efficiency.

General Health
A Complete Guide to Fatigue: Causes, Home Remedies, and Red Flags
Other than a hectic day, fatigue can also happen due to medical reasons! Read this blog, as we highlight the different causes, remedies and red flags of unexplained tiredness and when you should see a doctor.

General Health
Tired All the Time? Tests to Rule Out Underlying Illness
Constantly tired? Discover key blood tests for fatigue—thyroid, B12, Vitamin D, anaemia, and more. Book tiredness test packages online at Apollo 24|7.