Guide to Minimal Access Laparoscopic Surgery General Surgery/laparoscopic Surgery Has Evolved Know How
Explore this comprehensive guide to Minimal Access Laparoscopic Surgery. Understand how this key area of general surgery has evolved and its modern techniques.

Written by Dr. Md Yusuf Shareef
Reviewed by Dr. Shaik Abdul Kalam MD (Physician)
Last updated on 20th Feb, 2026
Guide to Minimal Access Laparoscopic Surgery General Surgery/laparoscopic Surgery Has Evolved Know How
Introduction
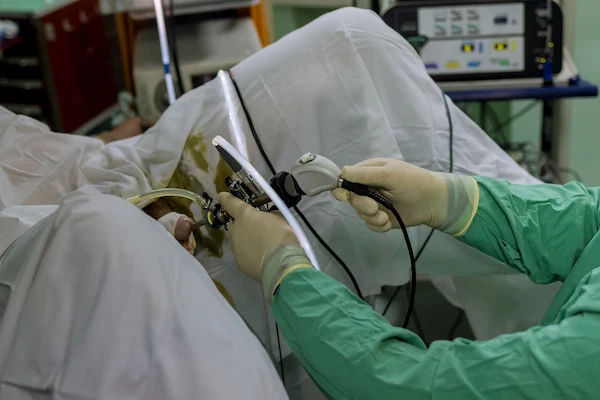
If you’ve heard terms like “keyhole surgery,” “minimally invasive,” or “minimal access laparoscopic,” they all point to a gentler way of operating—through tiny cuts rather than one large incision. Minimal access laparoscopic techniques use a pencil-thin camera and specialized instruments to diagnose problems and perform precise operations in the abdomen or pelvis. For many people, this means less pain, smaller scars, fewer complications, and a faster return to normal life than with traditional open surgery.
This guide is designed for the general public looking for clear, practical healthcare advice. We’ll break down how minimal access laparoscopic surgery works, its benefits and trade-offs, who makes a good candidate, and what to expect before, during, and after your operation. We’ll also cover the most common procedures, risks and prevention, recovery timelines, and how to choose the right surgeon and hospital. To help you decide confidently, we include evidence snapshots from trusted medical sources and add real-world tips you won’t find in most overviews. Whether you’re preparing for a gallbladder removal or just comparing options, this guide can help you discuss choices with your doctor and plan for a smoother recovery.
What “minimal access laparoscopic” really means
Minimal access laparoscopic surgery, often called “keyhole surgery,” is a form of minimally invasive surgery that uses small incisions (ports), a high-definition camera (laparoscope), and long, slim instruments to perform operations inside the abdomen and pelvis. Unlike open surgery, which relies on a large incision for direct access, the surgeon sees the operative field on a screen and manipulates instruments that pivot at the skin level. The abdomen is gently expanded with carbon dioxide (CO2) gas (insufflation) to create a safe working space.
Minimally invasive vs “minimal access” vs “keyhole” surgery
- Minimally invasive surgery (MIS) is the umbrella term that includes laparoscopy, thoracoscopy (chest), endoscopic
procedures, and robotic-assisted approaches. - Minimal access refers to the small incisions and specialized access devices used in laparoscopy.
- “Keyhole” is the lay term for the same approach—small cuts, less tissue disruption, and faster recovery.
How laparoscopy works: ports, camera, and CO2
- Ports are placed through 5–12 mm incisions. One port holds the camera; others hold working instruments.
- CO2 insufflation lifts the abdominal wall away from the organs, improving visibility and safety.
- Energy devices (e.g., ultrasonic shears, bipolar instruments) seal vessels and tissue, reducing bleeding.
- The operation is recorded on a monitor, aiding precision and allowing teams to review and improve performance over
time.
Unique insight: In experienced hands, the laparoscopic view can actually magnify and clarify anatomy better than the naked eye—important for fine tasks like bile duct identification during gallbladder surgery.
Benefits and trade-offs vs open surgery
For many operations, minimal access laparoscopic surgery offers well-documented advantages: less postoperative pain,
smaller scars, reduced blood loss, fewer wound infections, shorter hospital stays, and quicker return to normal activities
compared with open surgery [1-4]. Patients often report improved mobility on day one, and many procedures are now
day-care or next‑day discharge.
Evidence snapshot across common operations
- Gallbladder removal: Laparoscopic cholecystectomy typically enables faster recovery and fewer wound infections than
open surgery, with similar overall safety when performed by trained teams. - Appendectomy: Laparoscopic appendectomy is associated with shorter hospital stays and fewer wound infections, with
particular benefits for women of reproductive age and people with obesity. - Inguinal hernia repair: Laparoscopic approaches can reduce chronic groin pain and facilitate an earlier return to work
compared to open repair in many cases, especially for bilateral or recurrent hernias. - Colon surgery: Laparoscopic colectomy achieves comparable cancer outcomes to open surgery with faster recovery and
shorter length of stay when performed by experienced surgeons.
When open surgery may be safer or preferred
Open surgery remains essential in certain scenarios: unstable patients, complex adhesions from prior operations, severe
inflammation or perforation, or when visualization is unsafe. Sometimes surgeons “convert” from laparoscopic to open
mid-procedure to maintain safety—a sign of good judgment, not failure. Your surgeon should discuss the likelihood of
conversion and why it might be needed. Unique insight: Ask about your surgeon’s “conversion policy”—what
thresholds prompt conversion—to understand how they prioritize safety.
Common minimal access laparoscopic procedures
Gallbladder removal (cholecystectomy)
Laparoscopic cholecystectomy is the gold standard treatment for symptomatic gallstones. Small incisions allow removal of the gallbladder with minimal disruption. Many patients go home the same day; most return to normal light activities within a week. A key safety step is “critical view of safety,” a structured technique that confirms bile duct anatomy before cutting—adopted worldwide to reduce bile duct injuries [2-4]. Long-tail keyword to include naturally:
laparoscopic cholecystectomy recovery time. If gallbladder pain, fever, or jaundice persist beyond a few days, consult a
doctor online with Apollo 24|7 for further evaluation.
Appendectomy
Laparoscopic appendectomy offers faster recovery and fewer wound infections compared to open appendectomy, with similar or better outcomes for complicated appendicitis in many settings [3]. It’s particularly helpful when the diagnosis is uncertain; the camera can survey the abdomen to confirm appendicitis or find alternative causes of pain. Long-tail keyword: laparoscopic appendectomy recovery.
Hernia repairs (inguinal, ventral, umbilical)
For groin (inguinal) hernias, laparoscopic repair (TAPP/TEP) can reduce chronic pain and speed return to work,
especially for bilateral or recurrent hernias [5]. For ventral and umbilical hernias, laparoscopic or robotic approaches
can place mesh with smaller incisions, potentially lowering wound complications in people with obesity or diabetes.
Choice depends on hernia size, prior repairs, mesh considerations, and surgeon expertise.
Colon and metabolic/bariatric surgery
Laparoscopic colectomy treats conditions from colon cancer to diverticulitis, offering similar cancer control with shorter recovery [6]. Laparoscopic sleeve gastrectomy and gastric bypass (bariatric/metabolic surgery) are overwhelmingly
performed minimally invasively, reducing wound issues and enabling earlier mobility [7]. Long-tail keywords:
minimally invasive colon surgery outcomes; day care laparoscopic procedures (for select operations).
Are you a candidate? Evaluation, optimization, and planning
Who benefits most from laparoscopy
Most adults needing abdominal surgery can be considered for a minimal access laparoscopic approach. Benefits are
often pronounced for people with obesity (smaller wounds, fewer infections), those who need a quicker return to work,
and patients at higher risk for wound complications. Discuss goals: less pain, faster mobility, cosmetic concerns, or
reduced hospital time.
Situations where laparoscopy may not be advised
Factors that may limit a minimal access approach include severe cardiopulmonary disease (CO2 insufflation can affect
breathing/circulation), extensive prior abdominal surgeries with dense adhesions, severe inflammation/perforation, or unstable vital signs. Pregnant patients may still be candidates for laparoscopy in the second trimester with special precautions; decisions are individualized [1,2].
Pre-op tests, medications, and lifestyle optimization
Typical pre-op steps include blood tests (e.g., CBC, electrolytes), ECG, chest X-ray if needed, and imaging such as
ultrasound for gallbladder issues. Managing diabetes, stopping smoking, and optimizing nutrition reduce complications.
Clarify medication adjustments (e.g., blood thinners, diabetes drugs). Apollo 24|7 offers a convenient home collection
for tests like CBC, HbA1c, or vitamin D, which can be helpful during pre-op planning. If your symptoms do not
improve or you develop fever, jaundice, or persistent abdominal pain, consult a doctor with Apollo 24|7 for guidance.
On the day of your minimal access laparoscopic surgery
Anesthesia, positioning, and safety checks
Most procedures are done under general anesthesia. You’ll meet anesthesia staff to review your plan. In the operating
room, safety checklists (like WHO Surgical Safety Checklist) confirm your identity, the procedure, allergies, and
equipment readiness—these steps reduce preventable errors [1]. Body positioning is adjusted to help gravity move
organs away for better visibility; special padding protects nerves and pressure points.
Port placement, insufflation, and energy devices
The first port is placed (often near the navel), the abdomen is gently inflated with CO2, and additional small ports are
placed under camera guidance. The surgeon uses long instruments and energy devices to dissect and seal tissues while
watching a high-definition screen. Specimens are removed in protective bags. At the end, CO2 is released, ports are
closed, and local anesthetic may be used to reduce post-op pain. Unique insight: Ask whether your team uses “low-
pressure pneumoperitoneum” when possible—some studies associate it with less shoulder-tip pain and quicker recovery.
Risks, complications, and how teams reduce them
Any operation has risks. With minimal access laparoscopic surgery, serious complications are uncommon in
experienced hands, but it’s important to understand potential issues and how teams mitigate them.
Early risks (bleeding, infection, organ injury, clots)
- Bleeding and infection rates are generally lower than with open surgery due to smaller incisions.
- Organ or bile duct injury is rare but can occur; standardized techniques (e.g., critical view of safety for gallbladder
removal) reduce risk [2-4]. - Blood clots (DVT/PE) are prevented with early walking, compression devices, and blood thinners when needed.
- Gas-related discomfort (shoulder-tip pain) typically improves within 24–72 hours.
Late issues (hernia at port site, adhesions, chronic pain)
- Port-site hernias are uncommon and minimized by closing larger port sites carefully.
- Adhesions (internal scar tissue) can occur after any abdominal surgery; laparoscopy tends to reduce the risk compared
with open approaches. - Chronic pain is less common after laparoscopic hernia repair than after some open techniques, especially for inguinal
hernias [5].
Red flags after discharge and when to seek help
Call your care team or seek urgent care if you have fever over 38°C, worsening abdominal pain, persistent vomiting,
redness or pus at incisions, yellowing of eyes/skin, breathing difficulty, chest pain, or leg swelling. If symptoms persist
beyond two weeks or do not match your expected recovery, consult a doctor online with Apollo 24|7 or arrange a
physical visit for prompt assessment.
Recovery, rehab, and returning to normal life
Pain control, activity milestones, and diet
Expect mild-to-moderate pain at port sites and possible shoulder-tip discomfort from residual CO2. Pain typically
improves quickly; many patients use acetaminophen and anti-inflammatories with limited opioids if needed. Walking
the same day speeds bowel recovery and reduces clot risk. Clear liquids may be allowed within hours, advancing to
normal diet as tolerated for many procedures. Long-tail keywords: ERAS after laparoscopy; laparoscopic hernia repair recovery time.
Wound care, work/sport timelines, and travel
Keep incisions clean and dry; showering is often allowed within 24–48 hours (ask your surgeon). Light work may
resume in 3–7 days after simple procedures like appendectomy or cholecystectomy, with heavier lifting delayed 2–4
weeks. After hernia repairs, lifting restrictions are individualized—ask for written guidance. Air travel is possible once
you’re mobile, pain controlled, and cleared by your team—often within 1–2 weeks.
Enhanced Recovery After Surgery (ERAS) principles at home
ERAS protocols—carb-loading as allowed, multimodal pain control, early feeding and mobilization—shorten hospital
stays and complications [8]. At home, continue small frequent walks, hydrate, eat protein-rich foods, and follow your
bowel regimen if on opioids. Unique insight: Set “micro-goals” (e.g., 5-minute walk every 2 hours while awake) to build
momentum without overdoing it.
The future and your choices: tech, teams, and costs
Robotic surgery, single-incision, 3D/fluorescence, and AI
Robotic-assisted minimal access surgery can improve dexterity and 3D visualization. Single-incision laparoscopy (SILS)
hides scars within the navel but may trade off instrument triangulation. Fluorescence imaging (ICG) helps visualize bile
ducts or blood flow, potentially improving safety in certain procedures. AI-enabled video analysis is emerging to
enhance training and consistency. These tools are promising but benefits vary by procedure and surgeon experience;
outcomes depend most on the team’s skill and systems [1,2].
Choosing your surgeon and hospital: questions to ask
- How often do you perform this minimal access laparoscopic operation each year?
- What are your rates of conversion to open surgery and reasons for converting?
- How do you ensure bile duct identification (for gallbladder) or nerve preservation (for hernia)?
- Are you part of an ERAS program? What’s the expected recovery timeline for me?
- What complications should I watch for, and who do I call 24/7?
Unique insight: Ask if your team audits outcomes and participates in registries or quality programs—centers that measure performance tend to improve it.
Costs, insurance, and value-based decisions
Minimal access laparoscopic surgery can reduce length of stay and time off work, which may lower overall costs even if
operating room expenses are slightly higher in some settings. Insurance coverage varies; request a written estimate that
includes surgeon, anesthesia, hospital, and device fees (e.g., mesh). For planned procedures, compare facilities with
similar quality metrics. If financial constraints limit in-person consults, use an online second opinion to confirm the
plan; Apollo 24|7 can connect you to specialists and facilitate lab testing logistics.
Quick takeaways
- Minimal access laparoscopic surgery uses tiny incisions and a camera to deliver safe, effective operations with faster recovery for many conditions.
- Benefits include less pain, lower wound infection risk, shorter hospital stay, and quicker return to normal life compared
with open surgery. - Not everyone is a candidate; your health, prior surgeries, and the specific condition guide the best approach.
- Ask about your surgeon’s case volume, ERAS program, conversion thresholds, and 24/7 post-op support.
- Early walking, good pain control, and nutrition are key to recovery; know red flags and when to seek help.
- New tech (robotics, fluorescence, AI) is exciting, but team experience and quality systems matter most.
- If symptoms persist or recovery seems off-track, consult a doctor online with Apollo 24|7; for pre-op labs, consider
Apollo 24|7’s home collection services.
Conclusion
Minimal access laparoscopic surgery has transformed general surgery by making many operations safer, gentler, and
faster to recover from. For common needs like gallbladder removal, appendectomy, hernia repairs, and even colon procedures, the keyhole approach often means smaller scars, less pain, fewer infections, and a quicker return to work and family life. That said, the right approach for you is personal. It depends on your health, anatomy, prior surgeries, and the specific operation you need. The best outcomes come from experienced teams who apply consistent safety steps (like the critical view of safety), follow ERAS protocols, and know when to convert to open surgery to keep you safe.
As you plan, ask informed questions, align the plan with your goals, and prepare your home and schedule for recovery. If you’re comparing options or want a second opinion, connect with trusted clinicians. If symptoms persist beyond a couple of weeks or your recovery doesn’t match expectations, consult a doctor online with Apollo 24|7 or book a physical visit for timely evaluation. For pre-op labs like CBC or HbA1c, Apollo 24|7 offers a convenient home collection to streamline your preparation. With the right information and team, minimal access laparoscopic care can help you get well—and get back—to what matters most, sooner.
Consult a Top General Surgeon
Consult a Top General Surgeon

Dr. Balachandar Kariappa Reddy
General Surgeon
16 Years • MBBS, DNB (Gen. Surg.), FMAS.,FAIS
Chennai
Apollo Hospitals Greams Road, Chennai
(75+ Patients)

Dr Anubhav Chittari
General Surgeon
3 Years • MBBS, M.S GENERAL SURGERY
Bengaluru
PRESTIGE SHANTHINIKETAN - SOCIETY CLINIC, Bengaluru

Dr Venu Kumar K N
Vascular Surgeon
10 Years • MBBS, MS (Surg), DNB (Surg), M.Ch (Vas Surg), DrNB (Vas Surg)
Bengaluru
Apollo Clinic, JP nagar, Bengaluru

Dr. Rekha Jaiswal
General Surgeon
22 Years • MBBS, MS (Gen. Surg.), M.MAS (Master in Minimal Access Surgery), FIAGES, FMAS, FALS (Bariatric), DMAS & Robotic ( da Vinci), USA Trained- Bariatric & Robotic Surgery
Delhi
Apollo Hospitals Indraprastha, Delhi
(200+ Patients)

Dr. Sushil Kumar Jain
General Surgeon
31 Years • MBBS, MS (Surg.), HPBS, Cert CRS (England)
Delhi
Apollo Hospitals Indraprastha, Delhi
(75+ Patients)
More articles from General Medical Consultation
Frequently Asked Questions
What’s the difference between minimally invasive and minimal access laparoscopic surgery?
Both terms often refer to the same concept—small incisions with a camera and instruments. “Minimal access laparoscopic” specifies the abdominal approach using ports and CO2, sometimes called keyhole surgery.
How long is recovery after laparoscopic cholecystectomy?
Most people return to light activities within a week and to normal routines in 1–2 weeks. Lifting restrictions may last 2–4 weeks. Always follow your surgeon’s specific plan. Long-tail keyword: laparoscopic cholecystectomy recovery time.
Is robotic surgery better than standard laparoscopy?
It depends on the operation and the team. Robotics can improve dexterity and 3D views, but outcomes are driven most by surgeon experience and protocols. For many procedures, standard minimal access laparoscopic techniques achieve excellent results.
Can I have a laparoscopy if I’ve had prior abdominal surgery?
Often yes, but dense adhesions may make a laparoscopic approach more complex or necessitate conversion to open. Your surgeon will review imaging, risks, and a plan tailored to your history. Long-tail keyword: risks of laparoscopy in obesity (also relevant if applicable).
What are the main risks I should know about?
Infections, bleeding, injury to nearby organs, blood clots, and anesthesia risks. Serious complications are uncommon in experienced hands. Know red flags: fever, worsening pain, vomiting, jaundice, chest pain, or leg swelling—seek care promptly. If symptoms persist, consult a doctor with Apollo 24|7.