- female
- 65 Years
- 20/02/2025
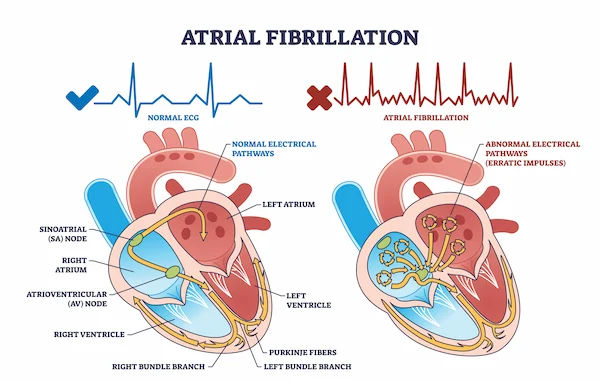
My mom's in the hospital with what's been diagnosed as an MUI heart attack. The doc's saying there's two blockages: one in the LAD that's 80% and another in the LCX at 99%. They've recommended doing angioplasty twicefirst for the LCX, then for the LAD. Is it really necessary to go through the procedure twice? Would love some advice on this.
Answered by 1 Apollo Doctors
In cases where multiple coronary arteries have significant blockages, it is not uncommon for doctors to perform angioplasty on separate occasions to address each blockage individually. This approach allows for better management of the procedure and reduces the risk of complications. It is important to follow the advice of your healthcare provider in this situation. The doctor may recommend starting with the LCX artery due to the higher percentage of blockage before proceeding to the LAD artery. The specific medications and dosages will be determined by the healthcare team based on your mother's individual condition.
Dr. Dhankecha Suggests...
Consult a Cardiologist
Answered 04/07/2025
0
0

More Cardiology Health Queries
View allI've been having this left upper chest pain along with a sensation of irritation or discomfort near the right side of my throat and towards the end of my molar teeth for the last 3-4 days. It's really worrying me. About 2 months ago, I had some heart tests done, but everything came back normal. I do have a BP of 14090 though and was taking TELMA H for two months. I quit smoking 6 months ago and used to smoke around 23 cigarettes a day. What could be causing these symptoms, and what should I do?
GERD take pantop 40mg for 3days
Answered by 1 Apollo Doctors
I'm curious about whether my resting heart rate is okay. I'm at 84 BPM, and I've read that's normal for my age and weight. Should I consider getting any further check-ups, or do you think it's all good?
cardiologist opinion
Answered by 1 Apollo Doctors
I have dental caries in 89 teeth and need extractions but I'm on Clopilet A 75 for my CAD with a stent. My dentist says to stop antiplatelet meds for a week before surgery but I'm not sure if it's safe. I take Metrogyl and Augmentin occasionally for infections and mostly eat soft foods. Can I really pause my antiplatelet meds for that long without risking my heart?
It's understandable to be concerned about stopping your antiplatelet medication. While some dentists recommend pausing antiplatelet drugs before dental extractions, it's generally not considered necessary, especially for procedures like extractions that have a low risk of bleeding. Dental extractions can be performed safely without stopping these medications as long as appropriate local hemostatic measures are taken.
Answered by 1 Apollo Doctors
Disclaimer: Answers on Apollo 247 are not intended to replace your doctor advice. Always seek help of a professional doctor in case of an medical emergency or ailment.


.webp)